Overview of PRP for Sports Injuries
PRP for sports injuries is a regenerative treatment approach that uses a patient’s own blood components to support healing in damaged tissues. This therapy concentrates platelets, which are rich in growth factors that play a key role in tissue repair and inflammation control. Athletes and active individuals often turn to PRP when dealing with persistent injuries that do not fully respond to rest or standard conservative care. It has become increasingly relevant in sports medicine due to its minimally invasive nature and biological approach to healing. Unlike traditional treatments that only manage symptoms, PRP for sports injuries focuses on enhancing the body’s repair processes. The treatment is widely used in orthopedic and sports rehabilitation settings for both acute and chronic conditions. Its growing popularity reflects the demand for alternatives to surgical intervention.
Common uses in athletic care
PRP for sports injuries is often recommended for soft tissue conditions that involve repetitive stress or overuse. These injuries typically affect tendons, ligaments, and muscles that are heavily engaged during physical activity. The treatment is particularly valued for its potential to improve healing quality in tissues with limited blood supply.
- Tendon inflammation and degeneration
- Ligament sprains and partial tears
- Muscle strain recovery support
- Joint irritation from repetitive motion
- Chronic overuse injuries in athletes
This approach is frequently chosen by individuals seeking non-surgical recovery options. It is also used as part of broader rehabilitation programs that include physical therapy and activity modification. The versatility of PRP for sports injuries makes it applicable across multiple athletic disciplines. Its use continues to expand as more clinical insights emerge.
Biological Mechanism Behind PRP Therapy
PRP for sports injuries works by concentrating platelets from a patient’s blood and delivering them directly to an injured area. Platelets contain bioactive proteins that signal the body to begin tissue repair. These growth factors stimulate cell regeneration, collagen production, and new blood vessel formation. This biological response helps accelerate healing in damaged tissues that typically recover slowly. The therapy essentially amplifies the body’s natural repair system in a targeted way. It is considered a regenerative medicine technique because it enhances structural healing rather than just symptom relief. The effectiveness depends on platelet concentration and injection accuracy.
Growth factors and healing response
The healing process triggered by PRP for sports injuries involves multiple biological signals working together. These signals help coordinate inflammation control and tissue regeneration at the injury site. The interaction between platelets and surrounding cells is essential for repair progression.
- Platelet-derived growth factor supports cell multiplication
- Transforming growth factor beta assists tissue remodeling
- Vascular endothelial growth factor promotes blood vessel formation
- Fibroblast activity increases collagen production
- Anti-inflammatory mediators reduce prolonged irritation
These elements work collectively to restore damaged tissue structure. The response varies depending on injury severity and location. In sports medicine, this mechanism is especially valuable for tendon and ligament healing. The controlled inflammatory phase is considered an important part of recovery.
Common Sports Injuries Treated with PRP for Sports Injuries
PRP for sports injuries is widely used for conditions that involve repetitive strain or trauma to soft tissues. These injuries are common among athletes who perform high-impact or repetitive movements. The therapy is often considered when standard rehabilitation has not produced sufficient improvement. It is also used to help reduce chronic discomfort associated with long-term overuse. Because of its regenerative potential, PRP is applied to both upper and lower body injuries. The treatment is tailored based on injury type and severity.
Frequently treated injury areas
Sports-related injuries treated with PRP often affect joints and connective tissues. These areas typically have limited blood flow, making natural healing slower.
- Shoulder tendon injuries including rotator cuff strain
- Knee conditions such as patellar tendon irritation
- Elbow pain commonly known as tennis elbow
- Achilles tendon inflammation in runners and athletes
- Muscle strains affecting hamstrings and quadriceps
These conditions are frequently seen in both recreational and professional sports. PRP for sports injuries is often integrated into recovery plans to support tissue repair. It is not limited to one sport or activity type. Its adaptability makes it a widely used option in orthopedic care.
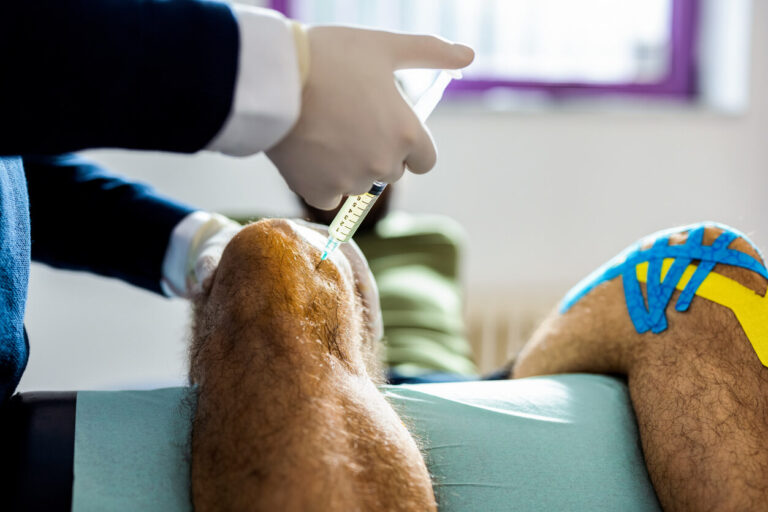
How PRP Therapy Is Performed
The process of PRP for sports injuries begins with a clinical evaluation to determine if the patient is an appropriate candidate. A small amount of blood is drawn and processed to separate platelet-rich plasma from other components. This concentrated plasma is then prepared for injection into the injured area. Medical imaging techniques may be used to ensure precise placement. The procedure is typically performed in an outpatient setting and does not require hospital admission. It is considered minimally invasive and usually completed within a short time frame. Patients are often able to return home shortly after the procedure.
Step-by-step process overview
The treatment process follows a structured approach to ensure safety and accuracy. Each stage is designed to maximize platelet concentration and delivery effectiveness.
- Blood sample collection from the patient
- Centrifugation to isolate platelet-rich plasma
- Preparation of concentrated plasma solution
- Image-guided injection into injury site
- Post-procedure observation and care instructions
This process is carefully controlled to maintain sterility and consistency. PRP for sports injuries relies heavily on proper preparation techniques. The precision of injection plays a key role in treatment outcomes. Medical supervision ensures that the procedure is safely performed.
Recovery Process After PRP for Sports Injuries
Recovery after PRP for sports injuries varies depending on the type and severity of the condition. Some patients may experience mild discomfort or swelling shortly after the injection. This response is considered part of the natural healing activation process. Over time, tissue repair gradually progresses as growth factors stimulate regeneration. Patients are often advised to modify activity levels during early recovery stages. Physical therapy is commonly incorporated to support functional improvement. The healing timeline may extend over several weeks or months.
What to expect during healing progression
The recovery journey following PRP for sports injuries involves gradual tissue rebuilding. Improvement is often seen in stages rather than immediate change.
- Mild soreness at injection site may occur initially
- Gradual reduction in pain and stiffness over time
- Improved joint or tendon function with rehabilitation
- Progressive return to physical activity levels
- Ongoing strengthening through guided exercise
These stages help ensure safe recovery without overloading healing tissues. Patients are encouraged to follow medical guidance closely. The combination of PRP and rehabilitation is often important for optimal results. Recovery patterns differ between individuals.
Benefits of PRP for Sports Injuries
PRP for sports injuries offers several potential advantages for individuals seeking non-surgical treatment options. It utilizes the body’s own biological material, reducing the risk of allergic reactions. The therapy is designed to enhance natural healing rather than replace it. Many patients appreciate its minimally invasive nature compared to surgical procedures. It is also commonly used when conservative treatments have not been fully effective. The regenerative approach is one of its most notable features. Its application continues to expand in sports medicine.
Key advantages in sports recovery
The benefits of PRP for sports injuries are closely tied to its biological mechanism and clinical application. These advantages make it a preferred option in many cases.
- Supports natural tissue regeneration
- Minimally invasive compared to surgery
- May reduce long-term pain in chronic injuries
- Enhances tendon and ligament healing response
- Uses patient’s own biological material safely
These benefits contribute to its growing use in athletic care. PRP for sports injuries is often part of a broader rehabilitation strategy. It is not a standalone solution but a supportive therapy. Its effectiveness depends on proper case selection.
Limitations and Considerations
PRP for sports injuries is not universally effective for all conditions. Some injuries respond better than others depending on severity and location. Variations in preparation techniques can also influence results. There is still ongoing research to standardize treatment protocols. Insurance coverage may not always include this therapy, making cost a consideration. Patients should maintain realistic expectations regarding outcomes. It is typically not an immediate fix but part of a longer healing process.
Important considerations before treatment
Understanding limitations helps patients make informed decisions about PRP for sports injuries. Not all cases are suitable for this approach.
- Results vary depending on injury type
- Multiple sessions may be required in some cases
- Protocols differ between medical providers
- Not suitable for all medical conditions
- Requires adherence to rehabilitation plans
These factors highlight the importance of medical evaluation. PRP for sports injuries should be considered within a comprehensive treatment plan. It is most effective when combined with structured rehabilitation. Individual response plays a significant role.
Who Are Ideal Candidates for PRP for Sports Injuries
PRP for sports injuries is generally recommended for individuals with specific types of musculoskeletal conditions. It is commonly used for patients who have not achieved full improvement through conservative treatments. Athletes with chronic overuse injuries often benefit from this approach. It is also suitable for active individuals seeking non-surgical options. Medical evaluation is necessary to determine eligibility. Age, health status, and injury type are important factors. The treatment is tailored to individual needs.
Suitable candidate profiles
Patients who may benefit from PRP for sports injuries often share similar characteristics related to injury patterns and activity levels.
- Individuals with chronic tendon pain
- Athletes with repetitive strain injuries
- Patients avoiding surgical intervention
- Active people with persistent joint discomfort
- Those unresponsive to standard therapy
These groups are commonly evaluated for PRP suitability. The decision is made based on clinical assessment. PRP for sports injuries is not a universal solution but a targeted therapy. Proper selection improves effectiveness.
PRP Compared with Other Sports Injury Treatments
PRP for sports injuries is often compared with other treatment methods such as corticosteroid injections, physical therapy, and surgery. Unlike corticosteroids, which mainly reduce inflammation, PRP focuses on tissue repair. Physical therapy supports movement and strength but may not directly accelerate biological healing. Surgery is typically reserved for severe cases but involves longer recovery time. PRP offers a middle ground between conservative and surgical approaches. Its regenerative focus makes it unique among treatment options. Choice of therapy depends on injury severity and patient goals.
Comparison points in treatment approaches
Understanding differences helps clarify where PRP for sports injuries fits in clinical care. Each method has distinct roles in recovery.
- PRP supports biological healing processes
- Corticosteroids mainly reduce inflammation
- Physical therapy improves mobility and strength
- Surgery repairs structural damage directly
- Stem cell therapy is still emerging in sports medicine
These distinctions guide treatment planning. PRP for sports injuries is often combined with other therapies. It is not always used alone. Its role depends on clinical judgment.
Risks and Possible Side Effects
PRP for sports injuries is generally considered safe due to its autologous nature. However, some mild side effects may occur following treatment. These are typically temporary and resolve without intervention. Infection risk is minimal when proper sterile techniques are used. Patients may experience localized discomfort after injection. Medical supervision helps reduce complications. Most individuals tolerate the procedure well.
Possible post-treatment reactions
Understanding potential effects helps prepare patients for PRP for sports injuries. These responses are usually short-term.
- Mild swelling at injection site
- Temporary soreness or stiffness
- Slight bruising in treated area
- Short-term inflammation response
- Rare risk of infection
These effects are generally manageable. PRP for sports injuries remains a low-risk procedure when properly performed. Monitoring and follow-up care are important. Most patients recover without complications.
Cost Factors of PRP for Sports Injuries
The cost of PRP for sports injuries varies depending on several factors. Location, provider expertise, and injury complexity all influence pricing. Multiple sessions may increase overall expense. Since insurance coverage is limited in many cases, out-of-pocket costs are common. Despite this, some patients consider it a worthwhile investment compared to surgery. Pricing transparency varies across clinics. Financial planning is often part of treatment decisions.
Elements influencing treatment cost
Understanding cost structure helps patients evaluate PRP for sports injuries realistically. Several components contribute to total expense.
- Clinic location and facilities
- Number of injections required
- Severity of injury condition
- Use of imaging guidance
- Provider specialization level
These factors create variation in pricing. PRP for sports injuries is considered a premium regenerative treatment. Costs should be weighed against potential long-term benefits. Consultation helps clarify financial expectations.
Scientific Evidence and Clinical Research
Research on PRP for sports injuries continues to grow in orthopedic and sports medicine fields. Studies show promising results for tendon-related conditions. However, outcomes vary depending on injury type and methodology. Some research supports improved healing in chronic tendon issues. Other studies highlight inconsistent results in certain applications. Ongoing clinical trials aim to refine treatment protocols. The scientific community continues to evaluate long-term effectiveness.
Current research insights
Scientific evaluation of PRP for sports injuries focuses on its regenerative potential. Evidence is still developing across different applications.
- Strong support for tendon injury improvement
- Mixed results in ligament recovery cases
- Growing use in sports medicine clinics
- Continued development of standardized methods
- Increasing interest in regenerative therapies
These findings highlight both potential and limitations. PRP for sports injuries remains an evolving treatment area. Further research will refine its clinical use. Evidence-based practice continues to guide application.
Recovery Optimization Strategies After PRP for Sports Injuries
Recovery following PRP for sports injuries can be improved through structured rehabilitation and lifestyle adjustments. Physical therapy plays a central role in restoring strength and mobility. Nutrition also supports tissue repair processes. Hydration and rest contribute to overall healing efficiency. Gradual return to activity helps prevent reinjury. Medical guidance ensures safe progression. Consistency in rehabilitation is important.
Supportive recovery practices
Optimizing recovery after PRP for sports injuries involves multiple supportive strategies. These enhance healing outcomes.
- Guided physical therapy sessions
- Protein-rich nutritional intake
- Controlled return to exercise
- Adequate rest and recovery periods
- Monitoring of pain and function levels
These practices help maximize treatment effectiveness. PRP for sports injuries works best when combined with structured rehabilitation. Patient compliance is essential. Recovery is a gradual process.
Frequently Asked Questions
What is PRP for sports injuries used for?
PRP for sports injuries is used to treat tendon, ligament, and muscle conditions that involve overuse or trauma. It supports natural tissue healing by using concentrated platelets from the patient’s blood.
How long does recovery take after PRP treatment?
Recovery time varies depending on injury severity, but improvements often occur gradually over several weeks. Some cases may take months for full tissue healing response.
Is PRP painful?
Most patients experience mild discomfort during or after injection, but it is generally well tolerated. Any soreness usually resolves within a short period.
How many sessions are needed?
Some patients may require a single session, while others benefit from multiple treatments depending on injury complexity.
Can PRP replace surgery?
In some mild to moderate cases, PRP for sports injuries may reduce the need for surgery, but severe structural damage may still require surgical intervention.
Takeaway
PRP for sports injuries represents a regenerative approach that supports the body’s natural ability to repair damaged tissues. It is widely used in sports medicine for tendon, ligament, and muscle conditions that require enhanced healing support. While it offers promising benefits, outcomes depend on proper diagnosis, technique, and rehabilitation adherence. Its role continues to grow as research advances in regenerative medicine and orthopedic care.