Understanding Sever Wound Surgery and Its Medical Importance
Sever wound surgery refers to specialized surgical procedures performed to treat deep, complex, and life-threatening injuries that involve extensive damage to skin, muscles, blood vessels, nerves, or even bones. This type of medical intervention is critical when ordinary wound care is not sufficient to restore tissue integrity or prevent serious complications. In many cases, sever wound surgery becomes necessary after accidents, violent trauma, or high-impact physical injuries. The primary goal is to stabilize the patient, prevent infection, and restore as much normal function as possible. Medical teams approach sever wound surgery with urgency because delayed treatment can lead to permanent disability or severe systemic infections. It is commonly performed in trauma centers where advanced surgical tools and multidisciplinary expertise are available. This type of surgery is not limited to closing wounds but also involves reconstructive techniques that rebuild damaged anatomy.
Sever wound surgery also plays an essential role in preventing long-term complications such as chronic pain, tissue necrosis, or loss of limb function. Surgeons carefully evaluate the extent of injury before deciding the best surgical approach. In many situations, multiple surgeries are required to fully restore the affected area. Patients undergoing sever wound surgery often require intensive post-operative care and long rehabilitation periods. The complexity of this medical field highlights its importance in emergency medicine and trauma care systems.
Types of Severe Wounds That Require Surgical Treatment
Severe wounds vary widely in their nature, but all require specialized surgical attention when tissue damage becomes extensive or life-threatening. Open deep lacerations are one of the most common injuries requiring sever wound surgery, where the skin and underlying tissues are cut deeply, exposing muscles or even bone. These injuries often involve significant bleeding and a high risk of infection, making immediate surgical repair necessary. Crush injuries are another serious category, usually caused by heavy objects compressing body parts, leading to extensive internal tissue damage and compromised blood flow.
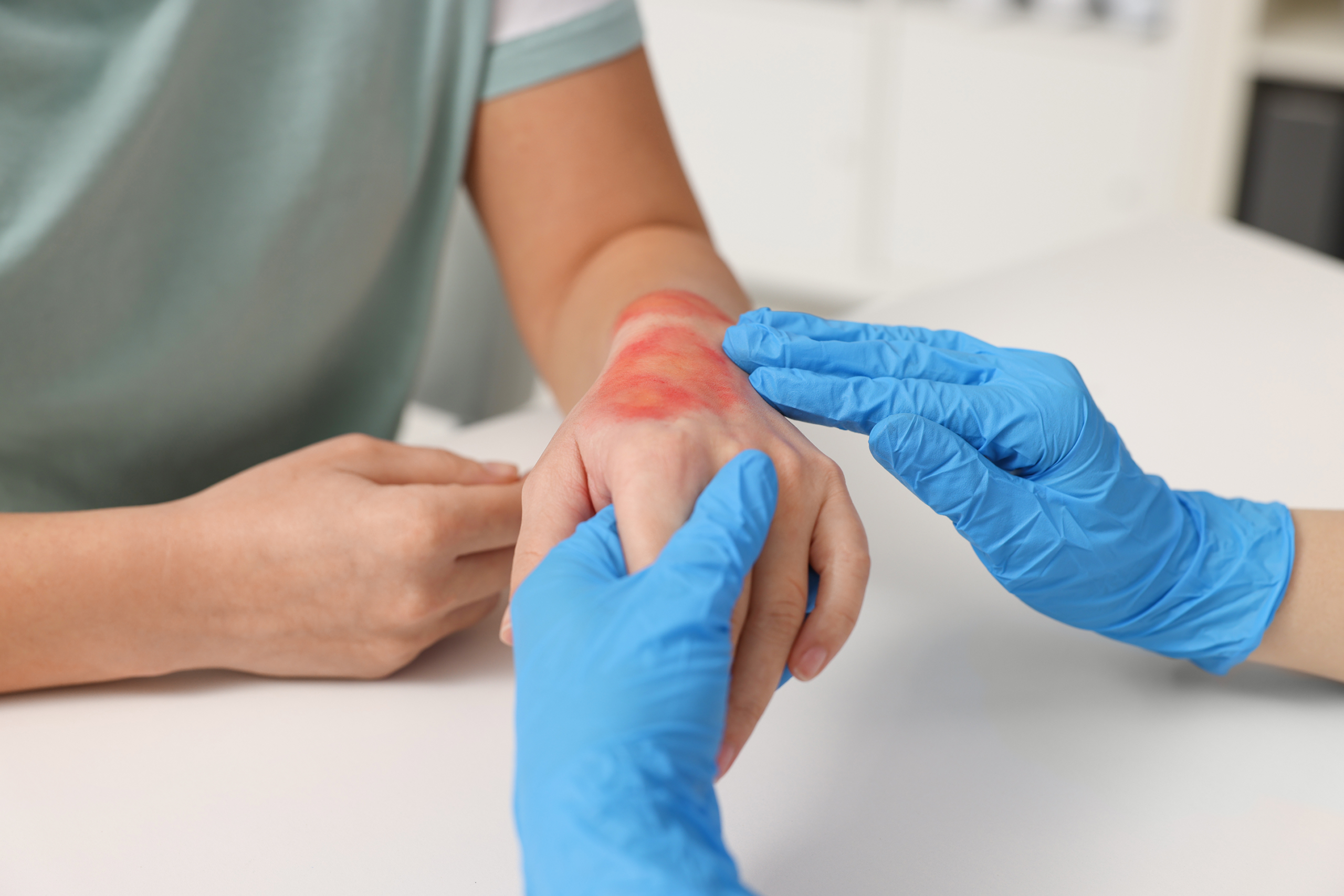
Avulsion injuries occur when skin or tissue is forcibly torn away from the body, often leaving irregular wound edges and exposed structures. These injuries are particularly complex because they require both wound closure and reconstructive procedures. Penetrating trauma, such as stab wounds or injuries caused by sharp objects, may damage internal organs and require immediate surgical exploration. Burn-related severe wounds also demand surgical intervention, especially when deep layers of skin are destroyed, requiring grafting or reconstructive techniques. Each type of wound presents unique challenges that influence the surgical approach and recovery process.
Initial Emergency Response Before Sever Wound Surgery
Immediate emergency response plays a vital role in improving outcomes before sever wound surgery is performed. The first priority is controlling bleeding, which may involve direct pressure, tourniquets, or emergency dressing techniques. Stabilizing the patient’s vital signs is also crucial, as severe blood loss can lead to shock and organ failure. Emergency medical teams often clean the wound superficially to reduce contamination before transferring the patient to surgical care. Rapid assessment ensures that life-threatening conditions are identified early and treated appropriately.
Diagnostic imaging such as X-rays, CT scans, and ultrasound is often used in emergency settings to determine the extent of internal damage. These tools help medical professionals understand whether bones, blood vessels, or internal organs are affected. Proper stabilization before surgery significantly improves survival rates and reduces complications during sever wound surgery. Emergency care also includes pain management and infection prevention measures to protect the patient’s condition while preparing for surgery. Every second counts in severe trauma cases, making emergency response a critical phase in treatment.
Diagnostic Process for Severe Wound Evaluation
Before performing sever wound surgery, a thorough diagnostic process is conducted to assess the full extent of injury. Physical examination is the first step, where doctors evaluate wound depth, tissue damage, and signs of infection. Circulation checks are performed to ensure that blood flow is not compromised in the affected area. In some cases, specialized imaging techniques are required to identify hidden injuries that are not visible externally.
Laboratory tests may also be ordered to detect infection markers or blood loss severity. Tissue viability assessments help determine which areas of damaged tissue can be saved and which must be removed during surgery. Accurate diagnosis is essential because it directly influences the surgical strategy used in sever wound surgery. The evaluation process also helps surgeons anticipate complications and prepare necessary medical resources. A detailed diagnostic phase ensures that surgery is both precise and effective.
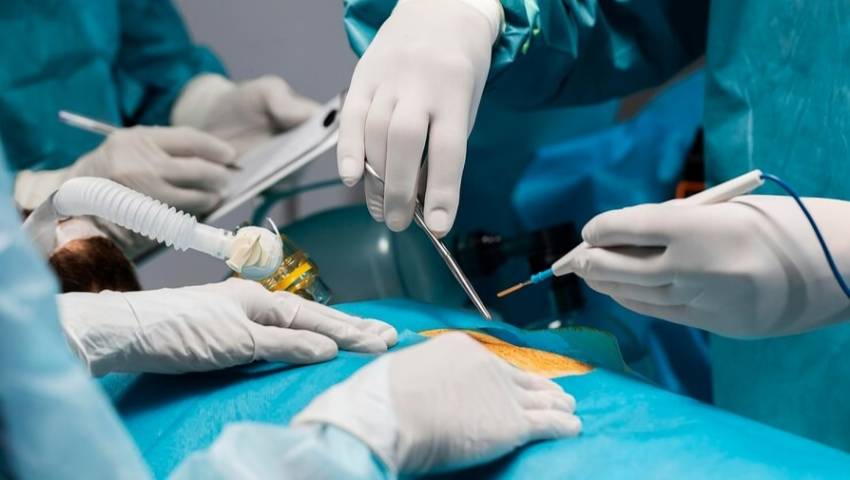
Surgical Procedures Involved in Sever Wound Surgery
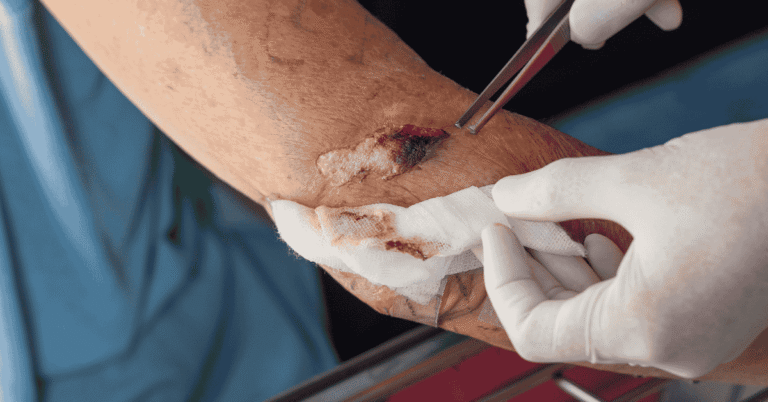
Sever wound surgery involves multiple surgical techniques depending on the severity and location of the injury. Debridement is one of the most important procedures, where dead or infected tissue is removed to prevent the spread of infection. This step is crucial for creating a clean environment for healing and reconstruction. Wound closure techniques such as suturing, stapling, or surgical adhesives are used depending on the wound type and severity.
Skin grafting is another key procedure, especially in cases where large areas of skin are lost. This involves transferring healthy skin from another part of the body or using synthetic substitutes. Reconstructive surgery is often required for complex injuries that affect muscles, nerves, or structural tissues. Microsurgery techniques allow surgeons to repair small blood vessels and nerves using high-precision instruments. These procedures collectively aim to restore both function and appearance as much as possible.
Anesthesia and Pain Management During Surgery
Anesthesia plays a critical role in ensuring patient comfort and safety during sever wound surgery. Depending on the severity of the injury, doctors may use local, regional, or general anesthesia. Local anesthesia numbs a specific area, while regional anesthesia blocks sensation in a larger part of the body. General anesthesia is used in more complex cases where the patient must remain unconscious throughout the procedure.
Pain management does not end after surgery, as post-operative care includes medications to control discomfort and inflammation. Monitoring the patient’s vital signs during surgery ensures that anesthesia is administered safely and effectively. Proper pain control also contributes to faster recovery and reduced stress on the body. Medical teams carefully adjust medication doses based on patient response. Effective anesthesia management is essential for the success of sever wound surgery.
Infection Control and Wound Sterilization Practices
Infection control is one of the most important aspects of sever wound surgery. Since severe wounds are highly susceptible to bacterial contamination, strict sterilization protocols are followed in operating rooms. Antibiotics are often administered before and after surgery to prevent infection development. Surgical instruments and environments are thoroughly sterilized to eliminate any risk of contamination.
Post-operative monitoring is also essential, as infections can develop even after successful surgery. Signs such as redness, swelling, or unusual discharge are carefully observed by medical staff. Maintaining a sterile environment significantly improves healing outcomes and reduces complications. Infection prevention strategies are integrated into every stage of sever wound surgery. This ensures patient safety and promotes faster recovery.
Recovery Process After Sever Wound Surgery
Recovery after sever wound surgery is a gradual process that requires medical supervision and patient cooperation. Immediately after surgery, patients are monitored closely to ensure stability and proper wound healing. Dressings are regularly changed to maintain cleanliness and prevent infection. Physical therapy may be introduced to restore movement and strength in affected areas.
Rehabilitation plays a significant role in long-term recovery, especially when muscles or joints are involved. Nutritional support is also important, as the body requires protein, vitamins, and minerals to rebuild tissue. Scar management techniques such as creams or laser therapy may be recommended depending on healing progress. Recovery timelines vary depending on the severity of the injury and the complexity of the surgery. Consistent follow-up care ensures optimal healing outcomes.
Potential Complications After Surgery
Although sever wound surgery is highly effective, certain complications may still arise during recovery. Infection remains one of the most common risks, especially in cases involving deep tissue damage. Delayed wound healing may occur due to poor blood circulation or underlying medical conditions. Tissue necrosis is another serious complication where damaged tissue fails to recover properly.
Nerve damage can result in temporary or permanent loss of sensation in the affected area. Blood clots may also develop, posing additional health risks if not treated promptly. Surgeons take preventive measures to minimize these risks, but patient monitoring remains essential. Early detection of complications significantly improves treatment outcomes. Understanding these risks helps patients stay informed and cautious during recovery.
Long-Term Outcomes of Sever Wound Surgery
Long-term outcomes of sever wound surgery depend on several factors, including injury severity and quality of post-operative care. Many patients regain significant physical function after successful treatment and rehabilitation. However, some may experience lasting effects such as scarring or reduced mobility. Reconstructive procedures can greatly improve both function and appearance over time.
Psychological recovery is also an important aspect, as traumatic injuries can affect emotional well-being. Ongoing medical evaluations help ensure that healing progresses as expected. Advances in surgical techniques have significantly improved long-term results in recent years. Patients are encouraged to maintain healthy lifestyles to support recovery. Overall, sever wound surgery offers strong potential for restoring quality of life.
Advances in Sever Wound Surgery Technology
Medical advancements have greatly improved the effectiveness of sever wound surgery in recent years. Robotic-assisted surgical systems allow for greater precision in complex procedures. 3D imaging technology helps surgeons plan operations more accurately by visualizing internal structures. Bioengineered skin substitutes are now used in cases where natural grafts are not available.
Regenerative medicine is also playing an increasing role in tissue repair and healing. New surgical materials provide stronger and more flexible wound closure options. These innovations have significantly reduced recovery times and improved patient outcomes. Continuous research continues to enhance the field of trauma surgery. Technology remains a key driver in improving sever wound surgery success rates.
Preventive Measures to Avoid Severe Wounds
Preventing severe injuries is always better than undergoing complex surgical treatment. Workplace safety measures such as protective gear can significantly reduce accident risks. Road safety practices, including seatbelt use and cautious driving, help prevent traumatic injuries. Sports activities should be performed with proper equipment and training to avoid injury.
Home safety also plays a role, especially in preventing falls or sharp object injuries. Awareness and education are key factors in reducing the occurrence of severe wounds. Employers and communities must promote safety standards consistently. Prevention strategies significantly lower the need for emergency surgical intervention. Maintaining caution in daily activities can help avoid life-threatening injuries.
When to Seek Immediate Medical Attention
Immediate medical attention is necessary when severe wounds occur, especially if bleeding cannot be controlled. Deep wounds exposing muscle, bone, or internal structures require urgent evaluation. Signs of shock, such as dizziness or rapid heartbeat, indicate a medical emergency. Severe pain or loss of sensation may suggest nerve involvement or serious tissue damage.
Foreign objects embedded in the body should never be removed without medical supervision. Delaying treatment can significantly worsen outcomes and increase complication risks. Emergency care facilities are equipped to handle such critical situations. Quick action can make a significant difference in recovery success. Recognizing warning signs helps ensure timely intervention.
Frequently Asked Questions (FAQ)
What is sever wound surgery used for?
Sever wound surgery is used to treat deep, complex injuries that cannot heal properly through basic wound care. It addresses damage to skin, muscles, nerves, and sometimes bones. The goal is to restore function and prevent complications such as infection or tissue death. It is commonly performed in trauma centers after accidents or serious injuries. Surgical techniques vary depending on wound severity. Each case is evaluated individually to determine the best approach. This type of surgery is essential in emergency medical care.
How long does recovery take after sever wound surgery?
Recovery time varies depending on the severity of the injury and the type of surgery performed. Some patients may recover within a few weeks, while others require several months of rehabilitation. Healing also depends on overall health and adherence to medical advice. Physical therapy may be necessary to restore movement and strength. Regular follow-up appointments are important to monitor progress. Complications can extend recovery time if they occur. Proper care significantly improves healing speed.
Is sever wound surgery painful?
Pain during sever wound surgery is controlled using anesthesia, so patients do not feel pain during the procedure. After surgery, some discomfort is expected as the body heals. Pain management medications are prescribed to help control this. The level of pain depends on the extent of the injury and surgery. Most patients experience gradual improvement over time. Medical teams closely monitor pain levels during recovery. Proper care ensures that discomfort remains manageable.
What are the risks involved in sever wound surgery?
Risks include infection, delayed healing, nerve damage, and blood clots. In some cases, additional surgeries may be required for full recovery. Tissue complications can also occur depending on injury severity. Medical teams take preventive measures to reduce these risks. Careful monitoring helps detect complications early. Patient health conditions can also influence risk levels. Despite risks, surgery is often necessary to save function or life.
Can all severe wounds fully heal after surgery?
Not all severe wounds heal completely, but many patients experience significant recovery. Healing depends on injury depth, location, and overall health condition. Reconstructive procedures can improve both appearance and function. Some patients may have lasting scars or minor limitations. Rehabilitation plays an important role in improving outcomes. Medical advancements have greatly improved healing success rates. Each case is unique in its recovery potential.
What is the difference between wound stitching and reconstructive surgery?
Wound stitching is a basic procedure used to close minor or moderate wounds using sutures. Reconstructive surgery is more complex and involves repairing damaged tissues, muscles, or structures. It is used in severe injuries where simple closure is not enough. Reconstructive procedures may include grafts or microsurgery techniques. The goal is to restore both function and appearance. Stitching is often the first step in wound care. Severe cases require advanced surgical intervention.
How can infection be prevented after surgery?
Infection prevention includes proper wound care, antibiotics, and maintaining cleanliness. Regular dressing changes are essential for keeping the wound sterile. Patients should follow all medical instructions carefully. Avoiding contamination and monitoring for symptoms is important. Hospitals use strict sterilization procedures during surgery. Early detection of infection signs improves treatment outcomes. Proper hygiene significantly reduces infection risk.
Are skin grafts permanent after sever wound surgery?
Skin grafts are generally long-lasting and become part of the body after healing. However, they may require time to fully integrate and function normally. Some grafts may change in texture or appearance over time. Proper care improves their durability and effectiveness. In some cases, additional procedures may be needed. Grafts help restore coverage and protect underlying tissues. They are a common and effective part of severe wound treatment.
Takeaway
Sever wound surgery plays a vital role in treating life-threatening injuries that involve deep tissue damage and complex trauma. It combines emergency care, advanced surgical techniques, and long-term rehabilitation to restore function and improve patient outcomes. Early intervention and proper medical treatment significantly increase the chances of recovery. Advances in surgical technology continue to improve precision, healing speed, and overall success rates.