Understanding Corneal Transplant
A corneal transplant, also known as keratoplasty, is a surgical procedure aimed at replacing a damaged or diseased cornea with healthy donor tissue. The cornea is the clear, dome-shaped surface that covers the front of the eye and plays a critical role in focusing light for sharp vision. Damage to the cornea from injury, infection, or genetic conditions can lead to blurred vision, severe discomfort, or even vision loss. Corneal transplant surgery restores both clarity and function to the eye, allowing patients to regain their quality of life. There are several types of corneal transplants, each suited to specific conditions. Penetrating keratoplasty replaces the full thickness of the cornea, while lamellar keratoplasty involves only the affected layers. Endothelial keratoplasty, including DSEK and DMEK, focuses on the innermost layer, providing faster recovery and fewer complications. Understanding these options helps patients make informed decisions with their ophthalmologist.
Conditions That Require Corneal Transplant
Corneal transplants are recommended for patients whose corneas are severely damaged or diseased. One common condition is keratoconus, a progressive thinning of the cornea that leads to vision distortion and irregular astigmatism. Corneal scarring due to infections like herpes simplex or bacterial keratitis can also necessitate a transplant to restore clear vision. Patients with corneal dystrophies, such as Fuchs’ endothelial dystrophy, often experience swelling and foggy vision, making surgery essential. Severe corneal edema or swelling caused by prior eye surgeries may compromise vision over time. Trauma, chemical burns, or accidents can lead to permanent corneal damage requiring replacement. Additionally, previous failed corneal surgeries may require a secondary transplant to correct vision problems. Identifying the underlying condition early ensures timely intervention and a higher likelihood of successful visual recovery.
Preparing for Corneal Transplant Surgery
Proper preparation is essential to the success of a corneal transplant. Patients undergo comprehensive eye examinations to assess overall eye health and determine the suitability of a transplant. Imaging tests such as corneal topography or optical coherence tomography help map the cornea and identify the extent of damage. Selecting the right donor cornea is another crucial step, with factors like tissue quality, age of the donor, and compatibility influencing outcomes. Patients must also undergo a health evaluation to identify conditions that may affect healing, such as diabetes or immune disorders. Pre-operative instructions often include stopping certain medications, avoiding contact lenses, and arranging post-surgery support. Mental preparation and understanding the surgical process reduce anxiety and improve patient cooperation. Surgeons discuss realistic expectations and possible outcomes to ensure patients are well-informed before proceeding.
The Corneal Transplant Procedure
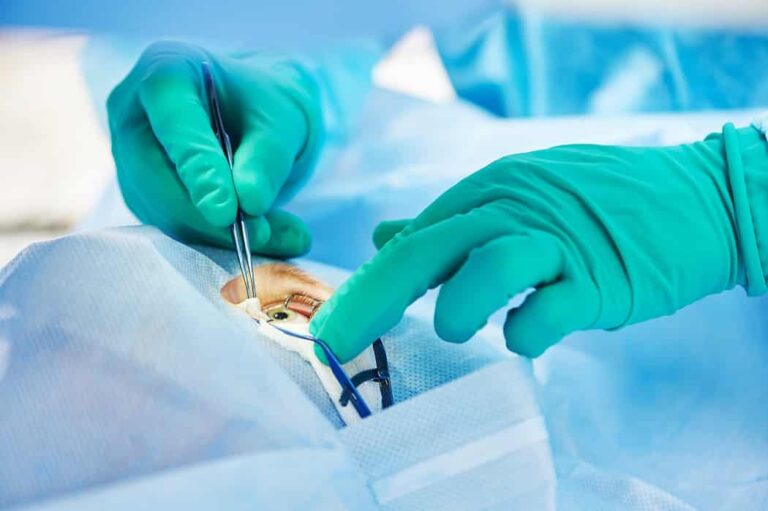
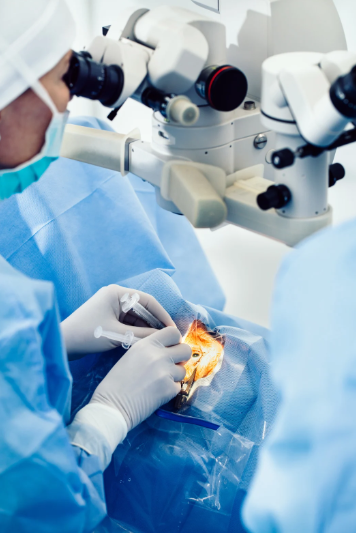
Corneal transplant surgery is performed with precision and care to restore vision effectively. The procedure typically begins with administering anesthesia, which may be local or general depending on the patient and type of transplant. The surgeon carefully removes the damaged corneal tissue and replaces it with a healthy donor cornea. In full-thickness transplants, the entire cornea is replaced, while partial-thickness procedures target only the affected layers. Specialized instruments ensure proper alignment and secure attachment of the donor tissue using tiny sutures or adhesive techniques. The surgery can take one to two hours, and most patients either go home the same day or stay briefly for observation. Immediate post-operative care includes monitoring eye pressure, applying protective eye shields, and taking prescribed medications to prevent infection and inflammation. Proper surgical technique and careful handling of the donor tissue are key to long-term graft survival.
Recovery and Post-Operative Care
Recovery after a corneal transplant requires patience and diligent care to ensure optimal outcomes. Patients may experience blurred vision, light sensitivity, or mild discomfort in the days following surgery. Eye drops are prescribed to prevent infection, reduce inflammation, and support healing. Protective eyewear may be recommended, especially during activities that risk eye injury. Regular follow-up visits allow the ophthalmologist to monitor graft health, detect early signs of rejection, and adjust medications as needed. The timeline for visual improvement varies depending on the type of transplant and individual healing. Lamellar and endothelial procedures often result in quicker recovery compared to full-thickness transplants. Maintaining good eye hygiene, avoiding strenuous activities, and adhering to medication schedules significantly increase the chances of a successful outcome.
Risks and Complications
Like any surgical procedure, corneal transplants carry potential risks that patients should understand. Common complications include infection, swelling, and the development of astigmatism that may require corrective lenses. Graft rejection, although relatively uncommon, is the most serious risk, occurring when the body’s immune system attacks the donor tissue. Symptoms of rejection may include redness, pain, light sensitivity, or sudden vision changes. Prompt recognition and treatment with medications such as corticosteroids are crucial for saving the graft. Rarely, the transplant may fail due to complications from the initial surgery, pre-existing eye conditions, or donor tissue issues. Patients can minimize risks by following post-operative care instructions closely and reporting any unusual symptoms immediately. Regular eye examinations for years after surgery ensure long-term graft health and vision stability.
Success Rates and Long-Term Outcomes
Corneal transplant surgery has a high rate of visual improvement when performed under proper conditions. Full-thickness transplants often restore functional vision in 70-90% of cases, while lamellar and endothelial procedures offer even faster recovery and reduced risk of rejection. Factors influencing success include the patient’s underlying eye condition, age, general health, and adherence to post-operative care. Visual improvement can continue for months to years, with some patients achieving near-perfect vision over time. Lifelong follow-up is recommended to detect early signs of complications and maintain graft health. Proper eye care, including avoiding trauma and managing systemic conditions like diabetes, supports long-term outcomes. Modern surgical techniques and tissue preservation methods have significantly improved both safety and success rates.
Innovations in Corneal Transplantation
Recent advances in corneal transplant techniques have revolutionized patient outcomes and recovery times. Endothelial keratoplasty, such as DMEK, involves replacing only the innermost corneal layer, resulting in faster visual recovery and fewer complications. Artificial corneas, or keratoprostheses, are increasingly used for patients unsuitable for traditional transplants. Advances in tissue preservation allow donor corneas to remain viable for longer periods, improving accessibility and success rates. Laser-assisted procedures enhance precision, reducing the risk of misalignment and post-operative astigmatism. Research into regenerative medicine, including stem cell therapy, shows promise for repairing damaged corneal tissue without full transplants. These innovations demonstrate the field’s commitment to improving both safety and patient quality of life.
Patient Experiences and Expectations
Understanding what to expect before and after a corneal transplant can ease anxiety and improve overall satisfaction. Patients may initially experience blurred vision and light sensitivity, which gradually improves with healing. Emotional responses, including relief, excitement, or anxiety, are common and should be acknowledged. Patient education about medication schedules, activity restrictions, and warning signs of complications helps manage expectations. Realistic goals, such as gradual improvement rather than immediate perfect vision, are important to communicate. Support from family, caregivers, and the medical team enhances recovery and adherence to care plans. Long-term lifestyle adjustments, such as protecting the eyes from trauma and maintaining general health, support graft longevity.
Frequently Asked Questions
How long does a corneal transplant last? Most corneal grafts last 10-20 years, although some may last a lifetime with proper care.
Is corneal transplant surgery painful? Most patients experience minimal pain, typically managed with over-the-counter medications or prescribed eye drops.
Can both eyes undergo transplant at the same time? Usually, only one eye is operated on at a time to reduce risk and allow proper healing.
What is the waiting time for a donor cornea? Waiting time varies depending on donor availability, often ranging from weeks to several months.
Are there alternatives to corneal transplant? In some cases, treatments like corneal cross-linking, specialized contact lenses, or keratoprosthesis may be considered.
Takeaway
Corneal transplant surgery has transformed the lives of countless patients by restoring vision and improving quality of life. Advances in surgical techniques, tissue preservation, and post-operative care make this procedure safer and more effective than ever. Understanding the process, potential risks, and recovery expectations helps patients make informed decisions. With proper preparation and adherence to follow-up care, a corneal transplant can provide long-lasting visual improvement. Patients are encouraged to maintain regular eye check-ups, protect their eyes, and consult their ophthalmologist promptly if any complications arise. This combination of modern medicine and patient diligence ensures the best possible outcomes for those seeking a brighter, clearer future through corneal transplantation.