Understanding Decubitus Ulcers and Why Proper Treatment Matters
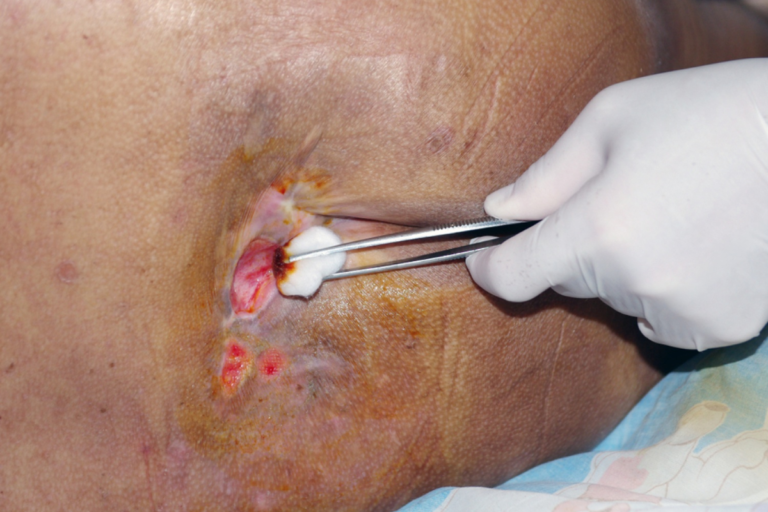
Decubitus ulcer treatment plays a critical role in preserving skin integrity, preventing infections, and improving overall quality of life for individuals with limited mobility. Decubitus ulcers, also known as pressure ulcers or bed sores, develop when prolonged pressure restricts blood flow to the skin and underlying tissues. This lack of circulation deprives cells of oxygen and nutrients, leading to tissue damage and eventual breakdown. Proper treatment is essential because these wounds can worsen quickly if not addressed early and consistently. Many people underestimate how rapidly a mild pressure injury can progress into a deep, infected wound. Without appropriate decubitus ulcer treatment, complications such as chronic pain, infection, and extended hospital stays may occur. Understanding the seriousness of these ulcers encourages timely care and proactive management.
Causes and Risk Factors That Influence Treatment Approaches
Effective decubitus ulcer treatment begins with identifying the causes and risk factors that contribute to wound development. Prolonged immobility is the most common factor, especially in individuals who are bedridden or wheelchair dependent. Poor circulation, often linked to conditions such as diabetes or vascular disease, also increases vulnerability to skin breakdown. Nutritional deficiencies play a significant role, as inadequate protein and calorie intake slow tissue repair. Aging skin is thinner and less elastic, making older adults more prone to injury. Moisture from perspiration or incontinence weakens the skin barrier and accelerates breakdown. Each of these factors influences how treatment plans are designed and adjusted. Addressing root causes allows healthcare providers to create more effective and sustainable treatment strategies.
Stages of Decubitus Ulcers and Corresponding Treatment Needs
Decubitus ulcer treatment varies significantly depending on the stage of the wound. Stage one ulcers present as reddened skin that does not blanch, requiring pressure relief and close monitoring. Stage two ulcers involve partial skin loss and often need protective dressings to maintain moisture balance. Stage three ulcers extend into deeper tissue layers and demand advanced wound care techniques. Stage four ulcers expose muscle or bone and require intensive medical intervention. Unstageable ulcers contain dead tissue that obscures the depth of damage. Deep tissue injuries may appear intact on the surface but deteriorate rapidly beneath. Accurate staging ensures that treatment matches the severity of the wound and prevents unnecessary complications.
Medical Assessment and Diagnosis for Effective Decubitus Ulcer Treatment
A thorough medical assessment is essential for guiding decubitus ulcer treatment. Healthcare providers evaluate the wound’s size, depth, and appearance to determine the extent of tissue damage. Signs of infection such as redness, warmth, swelling, or drainage are carefully documented. Pain levels and surrounding skin condition are also assessed to understand patient comfort and healing progress. In complex cases, imaging or laboratory tests may be used to detect deeper infection or bone involvement. Regular reassessment allows clinicians to adjust treatment plans as the wound evolves. Accurate diagnosis ensures that treatment remains appropriate and responsive. Ongoing evaluation is a cornerstone of successful wound healing.
Evidence Based Treatment Options for Decubitus Ulcers
Decubitus ulcer treatment relies on proven, evidence based interventions to promote healing. Pressure relief remains the foundation of care, achieved through repositioning schedules and support surfaces. Wound cleansing removes debris and reduces bacterial load, preparing the area for healing. Appropriate dressings help maintain moisture balance while protecting the wound from contamination. Debridement may be necessary to remove dead tissue that impedes healing. Pain management supports patient comfort and adherence to care plans. Together, these strategies form a comprehensive approach to wound care.
Core Elements of Effective Treatment
• Regular repositioning to relieve pressure
• Use of specialized mattresses and cushions
• Proper wound cleansing and dressing changes
• Removal of nonviable tissue when indicated
• Consistent pain management strategies
Each element contributes to faster healing and reduced risk of complications.
Advanced and Specialized Decubitus Ulcer Treatment Methods
Advanced decubitus ulcer treatment options are often required for severe or non healing wounds. Negative pressure wound therapy uses controlled suction to remove excess fluid and stimulate tissue growth. Biologic dressings and skin substitutes support regeneration in complex wounds. Hyperbaric oxygen therapy increases oxygen delivery to damaged tissues, enhancing healing potential. Surgical intervention may be necessary when conservative methods fail. These advanced treatments are typically coordinated by specialized wound care teams. Collaboration among healthcare professionals ensures that patients receive the most effective interventions available. Specialized care can significantly improve outcomes for challenging wounds.
The Role of Nutrition in Decubitus Ulcer Healing
Nutrition is a vital component of decubitus ulcer treatment and recovery. Protein is essential for tissue repair and collagen formation. Vitamins such as vitamin C and minerals like zinc support immune function and wound healing. Adequate hydration maintains skin elasticity and circulation. Malnourished patients often experience delayed healing and increased infection risk. Dietitians play an important role in assessing nutritional needs and recommending supplements. Ongoing monitoring ensures that nutritional support remains effective throughout treatment. A well balanced diet accelerates healing and strengthens overall health.
Infection Prevention and Management During Treatment
Preventing infection is a top priority in decubitus ulcer treatment. Open wounds provide an entry point for bacteria, increasing the risk of serious complications. Proper wound hygiene and sterile dressing techniques reduce contamination. Early detection of infection allows for prompt intervention. Antibiotics may be prescribed when bacterial involvement is confirmed. Caregivers must be educated on recognizing warning signs such as increased drainage or foul odor. Preventing infection protects both the wound and the patient’s overall health. Consistent infection control practices are essential for successful outcomes.
Preventive Measures to Support Long Term Treatment Success
Long term success in decubitus ulcer treatment depends on effective prevention strategies. Pressure redistribution through specialized equipment minimizes tissue stress. Daily skin inspections help identify early changes before wounds develop. Maintaining mobility, even through assisted movement, improves circulation. Education empowers patients and caregivers to take an active role in prevention. Personalized care plans address individual risk factors and lifestyles. Prevention reduces recurrence and supports lasting skin health. A proactive approach enhances treatment effectiveness and quality of life.
Home Care and Caregiver Involvement in Decubitus Ulcer Treatment
Home care plays a significant role in ongoing decubitus ulcer treatment. Caregivers must understand proper wound care techniques and repositioning methods. Creating a clean and comfortable environment supports healing. Monitoring for changes in the wound ensures timely medical attention when needed. Emotional support helps patients cope with discomfort and frustration. Clear communication with healthcare providers strengthens continuity of care. Informed caregivers contribute greatly to successful treatment outcomes. Home based care can be both effective and empowering.
Challenges in Decubitus Ulcer Treatment and How to Overcome Them
Decubitus ulcer treatment presents several challenges that require careful management. Delayed healing may occur due to underlying medical conditions. Patient discomfort can affect adherence to repositioning schedules. Limited resources may restrict access to advanced treatments. Recurrent ulcers require reassessment of prevention strategies. Interdisciplinary collaboration helps address these challenges effectively. Open communication among care teams ensures coordinated efforts. Overcoming obstacles leads to improved healing and reduced complications.
Frequently Asked Questions
What is the most effective decubitus ulcer treatment?
The most effective decubitus ulcer treatment combines pressure relief, proper wound care, nutritional support, and infection prevention. Treatment effectiveness depends on wound stage and individual risk factors. Early intervention significantly improves healing outcomes.
How long does decubitus ulcer treatment usually take?
Healing time varies depending on ulcer severity, overall health, and adherence to care plans. Mild ulcers may heal within weeks, while severe wounds can take months. Consistent treatment accelerates recovery.
Can decubitus ulcers heal without surgery?
Many decubitus ulcers heal with non surgical treatments such as dressings, pressure relief, and nutrition. Surgery is reserved for severe or non healing cases. Early care reduces the need for surgical intervention.
What signs indicate a pressure ulcer is worsening?
Increased pain, redness, swelling, drainage, or foul odor may indicate worsening. Fever or chills suggest systemic infection. Prompt medical evaluation is necessary.
How can caregivers help prevent recurrence?
Caregivers can prevent recurrence by maintaining repositioning schedules, monitoring skin daily, and ensuring proper nutrition. Education and vigilance are key to long term success.
Takeaway
Decubitus ulcer treatment requires a comprehensive, patient centered approach that addresses both healing and prevention. With proper care, education, and collaboration, even complex wounds can improve significantly. Early action, consistent management, and supportive caregiving make a meaningful difference in outcomes and quality of life.